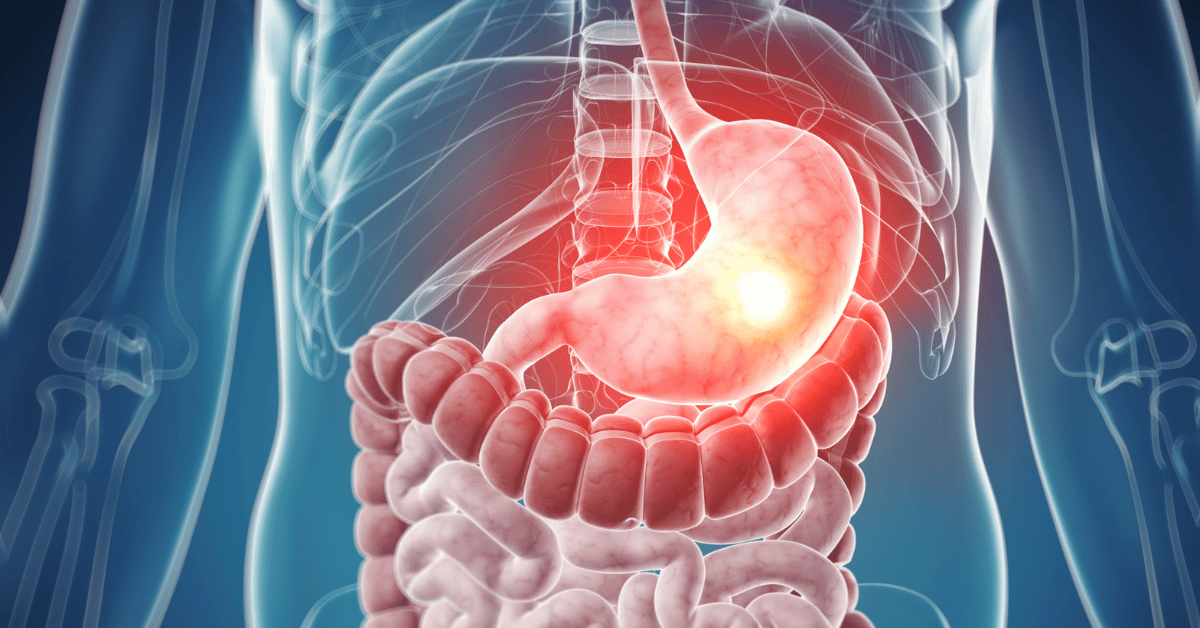
Gastroparesis refers to a condition in which the normal movement of food through the stomach to the small intestine is reduced significantly and stops in some instances. It disrupts the normal function of muscles in the stomach that contract and propel food in the direction naturally. This implies that food stays in the stomach for a more extended period than normal and induces discomfort and health complications.
This condition not only feels uncomfortable but also affects nutrition and blood sugar, which is more important in diabetic patients. With proper knowledge and early intervention, gastroparesis can be controlled and treated effectively.
Common Symptoms
Symptoms of gastroparesis are variable in severity and frequency. Nausea is one of the earliest to develop, and it often comes with frequent bouts of vomiting after consuming food. Fullness soon after ingesting in small quantities is a common experience of people with gastroparesis.
Bloating and upper abdominal pain are common, complicating the ability to handle normal portions of food. Acid reflux and consequent heartburn are sources of pain too.
Abrupt falls in blood sugar are frequent in diabetic patients with slowed digestion. Loss of appetite and unintentional weight loss are experienced when ingestion of food becomes troublesome with frequent regurgitation or persistent upper abdominal pains.
Root Causes
The causations of gastroparesis are numerous, but in certain cases, the causation remains unknown. Diabetes mellitus is one of the notable causes since high blood sugar damages the vagus nerve. This nerve controls the movement of muscles in the stomach.
Some surgeries on the stomach or adjacent nerve surgery can also introduce this condition. Some medications, such as opioids or some antidepressants, cause delayed gastric emptying as a side effect.
Neurological diseases such as Parkinson’s disease and multiple sclerosis are also causes of gastroparesis. Viral infections and autoimmune diseases, in some cases, interrupt the nerve output of the stomach and the muscle functions of the stomach.
Diagnosis Techniques
The diagnosis of gastroparesis consists of a complete medical history, physical assessment, and special testing. A gastric emptying study usually follows first because it can establish how quickly food exits the stomach. Upper endoscopy allows doctors to review the lining of the stomach and identify any flaws.
A barium X-ray or GI series is also a useful test because it traces the passage of food through the gastrointestinal tract. Gastric manometry also serves to measure the electrical and muscular activity of the stomach and inform doctors more about the condition.
Treatment Options
Treatment relies on the severity of the symptom and the reason. Dietary alterations, such as having small and frequent meals, are often recommended first. Not having fatty and fibrous food reduces strain on the stomach. Making sure to drink plenty of fluids also helps with digestion. Medications such as domperidone or metoclopramide that are prokinetic improve the contractions of the stomach, and antiemetics that prevent nausea and vomiting also improve these.
Severe cases may need to have gastric electrical stimulation or pyloroplasty performed. In extremely rare cases, feeding tubes are placed in the small intestine to provide nutrition.
Conclusion
Gastroparesis can be challenging but not impossible to manage through the right medical attention and lifestyle adjustments. Quality of life can be enhanced through early diagnosis and a personalised regimen of treatments. If you or a family member experiences recurrent gastrointestinal issues, Kaizen Hospital boasts extensive gastroenterology services, advanced diagnostic modalities, and customised treatments for conditions like gastroparesis.